GIRP notes

GIRP notes are a behavioral health progress note that can be used by clinicians to record treatment progress during a therapeutic session. GIRP stands for Goals, Intervention, Response, and Plan. GIRP notes are similar to other notes (e.g., SOAP and BIRP notes), except they emphasize achieving goals over analyzing client behavior. As such, you probably don’t want to use a GIRP note format unless the client is motivated to achieve a set of goals. Here is everything you need to know about GIRP notes.
Summary
- GIRP notes emphasize goal achievement over behavioral analysis, making them especially effective for motivated clients focused on progress. Each note includes four key components: Goals, Intervention, Response, and Plan. Download my free GIRP note template.
- The goals section should align with the treatment plan and use SMART criteria (Specific, Measurable, Achievable, Relevant, Time-bound). It focuses on what the client wants to achieve, both short- and long-term. Download my free SMART goals template.
- EHRs like TheraPlatform enhance GIRP documentation by offering customizable templates, HIPAA-compliant storage, note duplication, and integration with tools like Wiley Treatment Planners, streamlining therapist workflows.
Streamline your practice with One EHR
- Scheduling
- Flexible notes
- Template library
- Billing & payments
- Insurance claims
- Client portal
- Telehealth
- E-fax

Goals in GIRP notes
Goals are what sets GIRP notes apart from other similar notes. The emphasis is on what the client wants to achieve, rather than on a specific behavior or client experience. This section can include both short-term and long-term goals. More than any other type of note, it reflects the progress made on goals established in the treatment plan. When you fill out the goals section of a GIRP note, you should know what the client is working towards, both in the present and the future.
The goals section of GIRP notes should provide the answer to the following questions:
- What brought the client to therapy?
- What does the client want to work on?
- What do you think the client should be working towards?
Tips for writing the goals section of GIRP notes
- Use the SMART acronym as an effective tool for creating goals.
- Remark on both short-term and long-term goals.
- Make sure goals reflect the treatment plan.
- Don’t make goals that can’t be measured objectively.
Three examples of possible goals:
- John will build a more supportive social network as can be measured by the number of new friends (long-term).
- John will use cognitive restructuring to reduce anxiety by completing a daily thought record.
- John will reduce anxiety by performing one mindfulness exercise each day.
Practice Management + EHR + Telehealth
Manage more in less time in your practice with TheraPlatform

Intervention section of GIRP notes
The intervention section of GIRP notes state what methods are used to make the goals a reality. This part focuses on what the clinician did to work on the client’s objectives in the session.
The intervention section should provide the answer to the following questions:
- What interventions did the therapist use?
- How did the therapist help the client work towards achieving their goals?
- How were the client’s goals reflected in the intervention?
Tips for writing the intervention section of a GIRP note:
- A logical connection between goals and interventions should be evident.
- Action words (e.g., discussed, performed) are used to exhibit therapist interventions.
- Interventions should reflect the therapist’s theoretical orientation (e.g., CBT, psychodynamic).
- Don’t use an intervention that doesn’t fit your personal style, even if it sounds good.
Three examples of possible interventions:
- Therapist discussed with John realistic options for building a more supportive social network and decided on joining a new activity.
- Therapist explained the relevance of a thought record, showed John how to fill it out, and asked him to do so daily as homework.
- Therapist performed a guided meditation with John and directed him to an app to practice every day.
Response section of GIRP notes
The response section of GIRP notes detail the client’s response to the intervention. These responses should reflect the actual reaction in session, as well as client, reports as to their follow-through outside of treatment. This section is made up of both objective client behavior and subjective therapist interpretation.
The response section should provide the answer to the following questions:
- What is the client’s attitude toward therapy?
- Is the client making progress toward achieving their goals?
- Is the client struggling with any specific interventions?
Tips for writing the response section of a GIRP note:
- Use direct client quotes.
- Document physical observations of the client in session.
- Write down what interventions are working and those that are not.
- Don’t make interpretations that aren’t backed up by evidence.
Three examples of possible responses:
- John expressed hesitancy to go outside his comfort zone to participate in new social situations.
- John has been inconsistent in filling out daily thought records.
- John seemed receptive to mindfulness meditation and displayed evidence that he has been meeting his goals on the Headspace app.
Plan section of GIRP notes
The plan section of GIRP notes display the direction in which treatment is going.
It should provide the answer to the following questions:
- When is the date and time of the next session?
- Was the client assigned homework?
- What goals will be the focus of the next session?
Tips for writing the plan section of GIRP notes:
- Make sure the weekly GIRP notes plan reflects the overall client treatment plan.
- Note if the client has been referred to another specialist, such as for medication administration.
- Change up the plan if it isn’t working.
- Don’t ram homework down the client’s throat if they don’t consistently complete it.
Three examples of possible plans:
- The next therapy session with John is Thursday at 3 pm.
- John was assigned the task to continue daily mindfulness meditation.
- The therapist will explore John’s reluctance to complete thought record homework.
How EHRs can help with documentation
Modern EHR/practice management platforms (such as TheraPlatform) assist greatly with documentation by providing HIPAA‑compliant, integrated systems for note entry, storage, scheduling, and billing.
They allow therapists to:
- Use and customize templates (e.g., SOAP, DAP, and others) or build their own to streamline note writing and ensure consistency.
- Link notes to treatment plans, goals, and session history so client progress is easily tracked over time.
- Utilize e-fax and secure document sharing via client portal to safely exchange information with clients or other providers while maintaining confidentiality.
- Leverage dictation and telehealth transcription, which can automatically convert sessions into therapy or assessment notes, saving time and reducing manual entry.
- Take advantage of AI features that streamline documentation by automatically populating intake form data into assessment templates and generating complete therapy and assessment notes from the information you provide, all with a single click.
Watch this video to learn how to save time on therapy notes
Meanwhile, AI‑assisted note tools are emerging which can further help clinicians by:
- Automatically transcribing session audio (if permitted) and highlighting key moments (e.g. emotional shifts, major themes).
- Suggesting draft notes or filling in objective or assessment sections based on observed data, freeing up clinicians’ time.
- Supporting consistency and reducing missing components in notes, which helps from both clinical, legal, and insurance perspectives.
Together, structured SOAP‑type notes, good EHR platforms, and smart AI tools support better therapeutic outcomes, more efficient workflows, and stronger accountability.
GIRP notes example
Here is an example of a well-executed GIRP note for our client John, who is suffering from social anxiety.
Client: John Doe
Date: xx/xx/xxxx
Goals
- Long-term goal: John wants to build a more supportive social network. He feels isolated and lonely. He reports significant anxiety that keeps him from meeting new people and forming lasting relationships.
- Short-term goals: John will join one new activity in the next two weeks. He will perform cognitive restructuring daily to address anxiety. Finally, he will establish a regular mindfulness practice.
Intervention
This therapist discussed with John his reluctance to meet new people and how his anxiety appears to be impeding progress. We talked about realistic options to meet people and it was decided he would join one new activity in the next two weeks. Additionally, the rationale of a thought record was again explained to John and he was asked to complete one every day regarding his anxious thoughts. Finally, this therapist and John engaged in a guided mindfulness meditation aimed at decreasing anxiety. He was tasked with completing a daily meditation on his own using the Headspace meditation app.
Response
John appeared motivated to join a new activity. He stated that he understands he can’t make friends sitting in his apartment alone. Although John appeared to comprehend the CBT concepts behind reducing anxiety, he has not consistently completed his thought records. He has appeared much more invested and enthusiastic in mindfulness meditation. He has downloaded the app and begun to participate in daily meditations.
Plan
This therapist will meet with John again next Thursday at 3 p.m. He is to complete a daily mindfulness practice for next week. He was again assigned homework using thought records to address anxious thinking. If he doesn’t complete this assignment, his reluctance will be discussed and a new plan to address anxious thinking may need to be developed.
GIRP notes are a comprehensive and efficient platform for keeping track of client progress in a behavioral health setting. What sets them apart from other progress notes is the focus on the client’s goals.
Free Resources for Therapists
Click below and help yourself to peer-created resources:

How to improve GIRP notes with an EHR
Electronic Health Records (EHRs) have the potential to improve the efficiency and accessibility of GIRP (Goals, Interventions, Response, and Plan) notes in several ways. Integrating an EHR, alongside practice management software like TheraPlatform, can offer significant advantages to therapists in private practice:
Advantages of utilizing an EHR for GIRP Notes:
- Customizable templates streamline GIRP note creation: Some EHRs provide therapists with built-in templates for GIRP notes, simplifying the note-writing process. These templates can be tailored to meet the specific requirements of therapists' practices. Storing GIRP notes centrally in EHRs enhances accessibility.
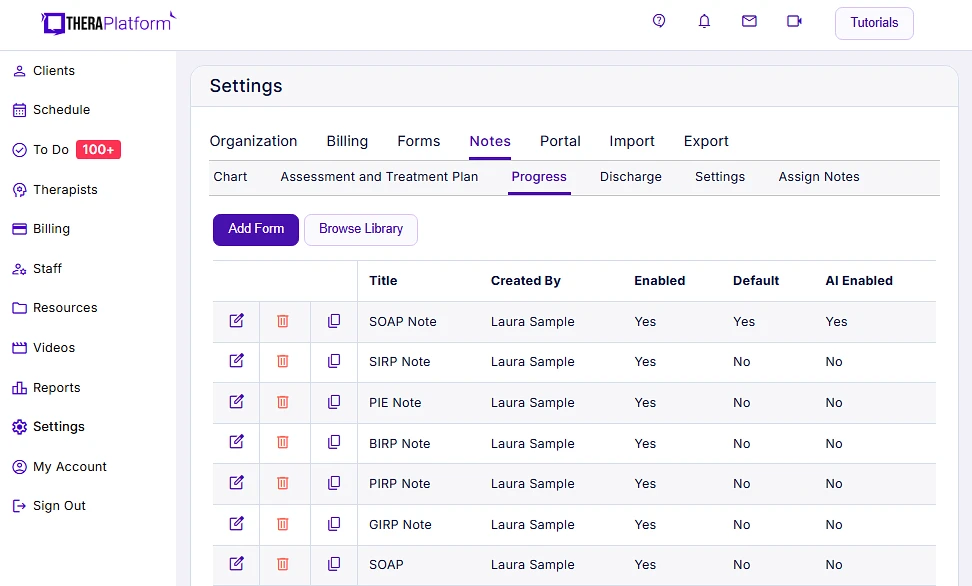
Screenshot of TheraPlatform's notes library.
- Flexible note template builder: Some EHRs offer a template builder that serves as a base for GIRP note documentation. These templates are populated with essential fields, enabling therapists to easily complete various sections of a GIRP note. Therapists can customize templates to align with their preferred documentation style. The intuitive template builder saves time and offers customization options.
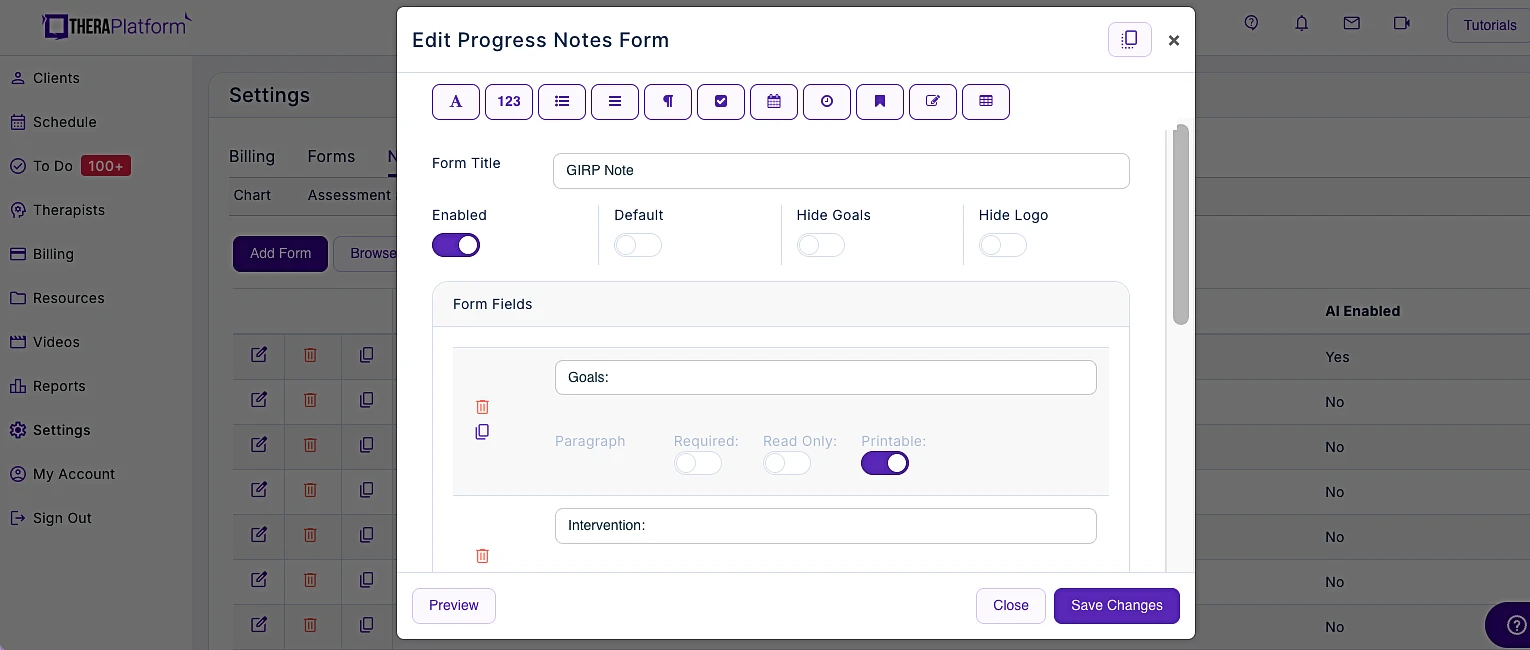
Screenshot of TheraPlatform's GIRP form builder. Use existing templates or create your own with new fields like pick lists, checkboxes, and buttons.
- HIPAA-Compliant Storage: TheraPlatform prioritizes the secure storage of GIRP notes by employing encryption and robust security measures. They also provide legally-binding Business Associate Agreements, ensuring compliance with HIPAA regulations for safeguarding Protected Health Information (PHI).
- Secure and convenient note sharing: GIRP notes may need to be shared for various reasons, including increasing transparency in mental health care, providing clients with insights into their progress, or for insurance purposes. EHRs facilitate secure and easy access to GIRP notes, saving time compared to traditional paper-based methods like manual retrieval or faxing.
- Integration with Wiley Treatment Planners: TheraPlatform integrates with Wiley Treatment Planners, enabling therapists to quickly access evidence-based treatment objectives, interventions, homework assignments, and diagnostic codes like ICD-10 and DSM-5. This integration streamlines treatment planning, saving therapists valuable time.
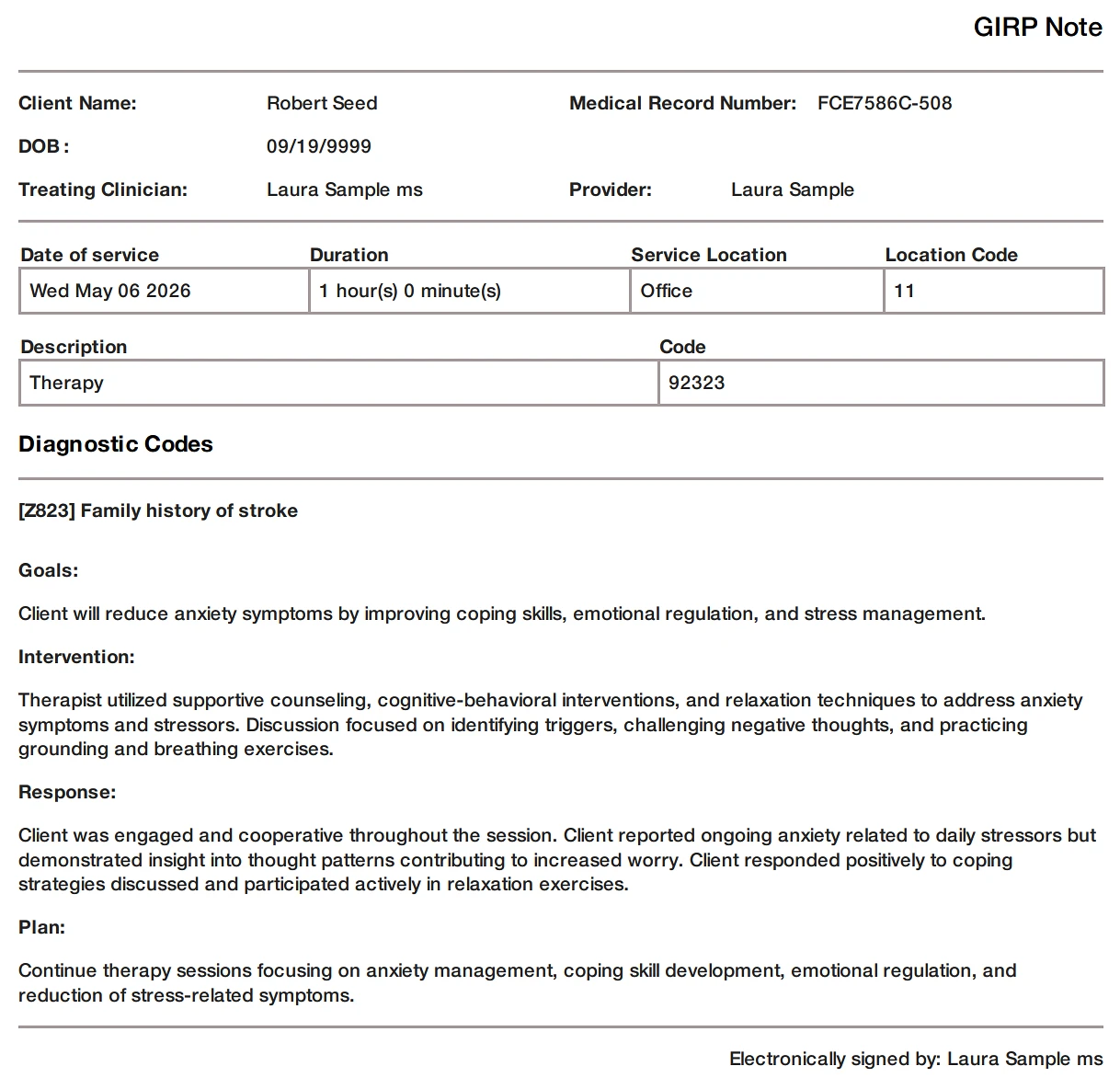
Example: TheraPlatform's screenshot of GIRP note created with TheraPlatform. Stay consistent with GIRP note taking with templates.
- GIRP Note duplication: While the content of GIRP notes may change from session to session, certain information can be repetitive. EHRs allow therapists to duplicate relevant notes and retrieve data from previous sessions. Homework assignments from earlier plans can also be carried over, and notes can be edited as needed.
- Effortless signatures: TheraPlatform's Pro and Pro Plus plans offer the convenience of requesting electronic signatures directly on notes. This feature is particularly useful when working with pediatric clients, as it allows for signatures from parents or legal guardians. Clients can easily download and print these documents as required.
- Efax Integration: TheraPlatform, an all-in-one EHR, practice management, and teletherapy solution, offers efax integration. This eliminates the need to switch between multiple services, saving time and reducing costs by enabling seamless sending and receiving of documents such as GIRP notes via efax directly within TheraPlatform. No more fighting with the fax machine!
Additional tools to help with data collection and progress monitoring for your GIRP notes
Therapists can also take advantage of EHRs (such as TheraPlatform) that offer integrations with Wiley treatment planners and built-in outcome measures to ensure consistent data collection on progress from session to session. The best part about partnering with a modern EHR is the time you save on formulating the actual notes and scoring.
What is Wiley Treatment Planner?
Wiley Treatment Planner is a widely used clinical resource designed to help mental health professionals and other therapists efficiently create treatment plans for their clients. In addition to treatment plans, the company also provides prewritten therapy notes for some diagnostic codes. It is part of the "PracticePlanners" series published by Wiley.
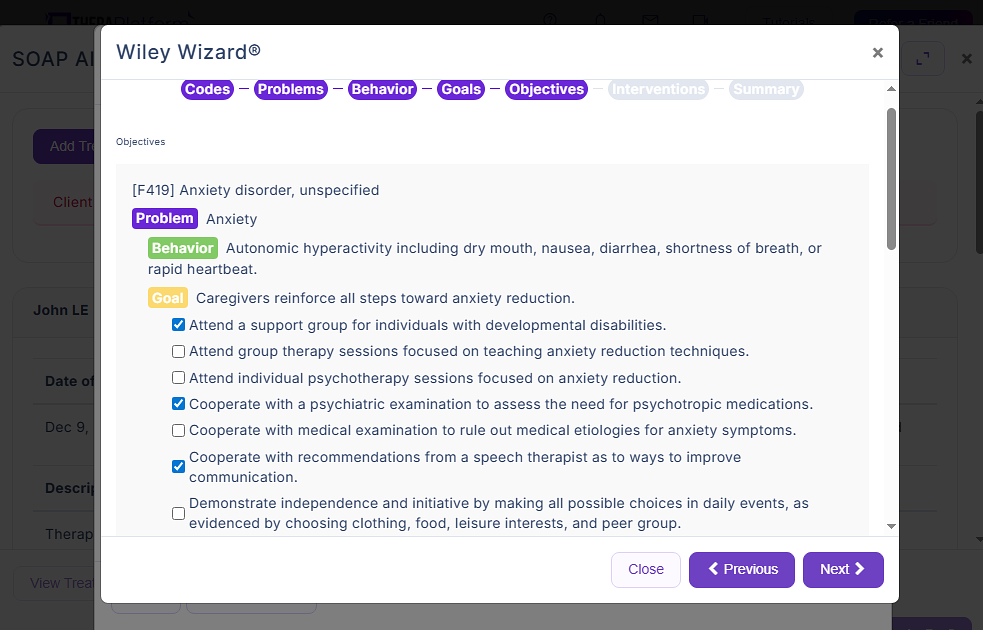
Screenshot of TheraPlatform’s Wiley Treatment Planner integration. Wiley offers thousands of prewritten, evidence-based treatment goals, objectives, and interventions for mental health therapists in private practice.
Features of Wiley Treatment Planner includes:
- Prewritten, evidence-based treatment goals, objectives, and interventions
- Treatment planners tailored to specific populations and problems, including adults, children, adolescents, couples, families, addictions, and more
- Alignment with the diagnostic criteria from the DSM-5 and ICD-10
- Prewritten therapy notes
Is there an online version of Wiley Treatment Planner and how can I get the Wiley Treatment Planner?
Wiley Treatment Planner company partnered with a select number of EHRs for mental health providers to make treatment planners available online. TheraPlatform’s EHR offers the Wiley Treatment Planner as an add-on for both assessment and treatment plans and therapy notes, such as DAP notes. You can edit prewritten notes and add your own with any therapy template on TheraPlatform.
Leveraging an EHR like TheraPlatform helps therapists enhance the quality and efficiency of their GIRP notes, streamline workflows, secure storage and easily access records.
Streamline your practice with One EHR
- Scheduling
- Flexible notes
- Template library
- Billing & payments
- Insurance claims
- Client portal
- Telehealth
- E-fax

Resources
Theraplatform is an all-in-one EHR, practice management and teletherapy solution that allows you to focus more on patient care. With a 30-day free trial, you have the opportunity to experience Theraplatform for yourself with no credit card required. Cancel anytime. They also support different industries including mental and behavioral health therapists in group practices and solo practices.
More resources
- Therapy resources and worksheets
- Therapy private practice courses
- Ultimate teletherapy ebook
- The Ultimate Insurance Billing Guide for Therapists
- The Ultimate Guide to Starting a Private Therapy Practice
Free video classes
- Free mini video lessons to enhance your private practice
- 9 Admin tasks to automate in your private practice
FAQs about GIRP notes
What are GIRP notes and when should therapists use them?
GIRP notes are a structured form of clinical documentation used in therapy to track client progress. GIRP stands for Goals, Interventions, Response, and Plan. They are especially useful for documenting goal-directed treatment, monitoring measurable progress, and supporting ongoing clinical decision-making with engaged, goal-oriented clients.
What should be included in each section of a GIRP note?
A GIRP note includes four sections: Goals (specific client treatment objectives), Interventions (therapist-led strategies or techniques used during the session), Response (client reaction, engagement, and measurable progress), and Plan (next steps, modifications, and future treatment direction).
How do EHRs help with GIRP notes?
EHR systems streamline GIRP note documentation by offering customizable templates, optional AI-assisted tools, note duplication features, secure storage, and integrated workflow tools. These features improve efficiency, reduce administrative burden, and support consistent, accurate clinical documentation.



